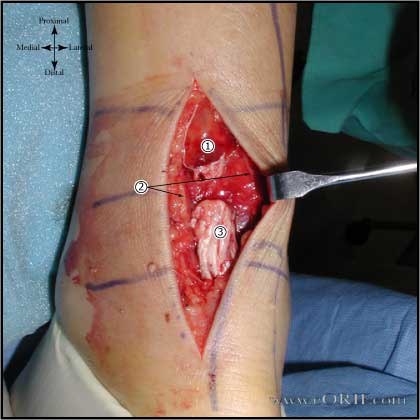
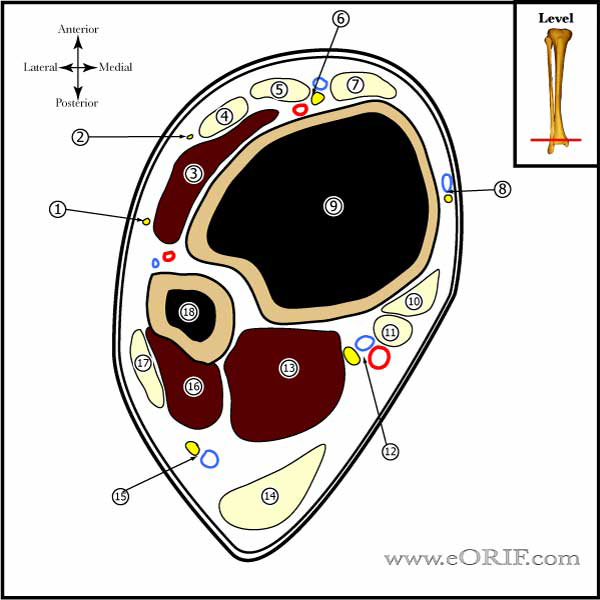
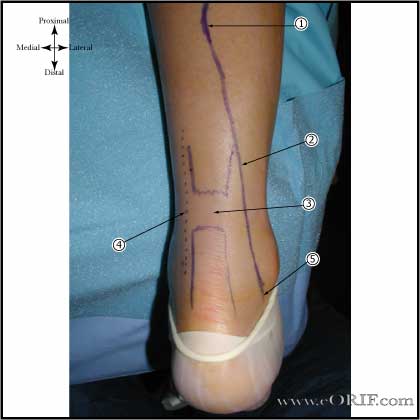
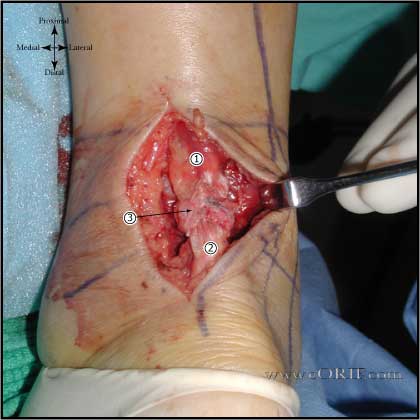
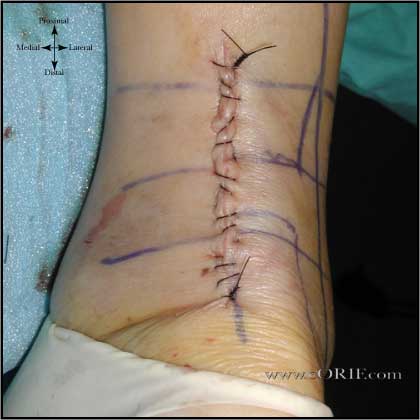
synonyms:Achilles tendon repair, gastrocnemius tendon repair, heel cord repair Achilles Tendon Repair Indications
Achilles Tendon Repair Contraindications
Achilles Tendon Repair Alternatives
Achilles Tendon Repair Pre-op Planning
Achilles Tendon Repair Technique
Achilles Tendon Repair Complications
Achilles Tendon Repair Follow-up care
Achilles Tendon Repair Outcomes
Achilles Tendon Repair Review References
|