|
|
Synonyms: Bankart tear, Bankart lesion, shoulder instability, glenohumeral instability, Perthes-Bankart lesion, shoulderarm Bankart, glenoid labral tear, glenoid labrum tear,
Bankart Lesion ICD-10 Glenoid labral tear ICD-10
- S43.491A Other sprain of right shoulder joint, initial encounter
- S43.492A Other sprain of left shoulder joint, initial encounter
- S43.82XA Sprain of other specified parts of left shoulder girdle, initial encounter
- S43.80XA Sprain of other specified parts of unspecified shoulder girdle, initial encounter
- S43.81XA Sprain of other specified parts of right shoulder girdle, initial encounter
- M24.111 Other articular cartilage disorders, right shoulder
- M24.112 Other articular cartilage disorders, left shoulder
- M24.119 Other articular cartilage disorders, unspecified shoulder
- M24.41 - Recurrent dislocation, shoulder
- M24.411 - Recurrent dislocation, right shoulder
- M24.412 - Recurrent dislocation, left shoulder
- M24.419 - Recurrent dislocation, unspecified shoulder
- See all Dislocation shoulder ICD-10 codes
- See all Instability shoulder ICD-10 codes
Bankart ICD-9
- 718.21= pathologic dislocation, shoulder region
- 718.31 = recurrent shoulder dislocation
- 905.6 = late effect of dislocation
- 905.7 = late effect of sprain/strain
Bankart Etiology / Epidemiology / Natural History
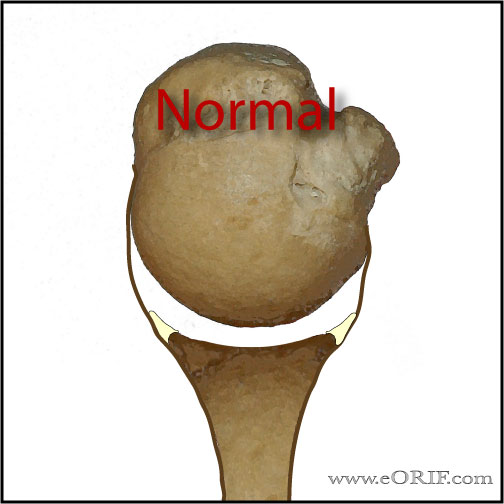
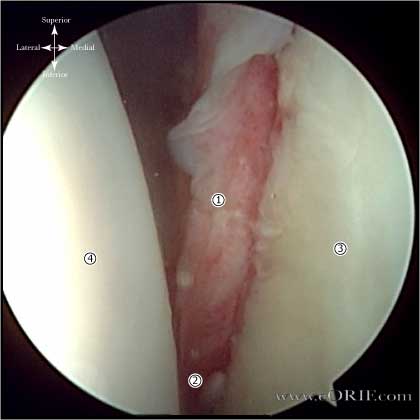
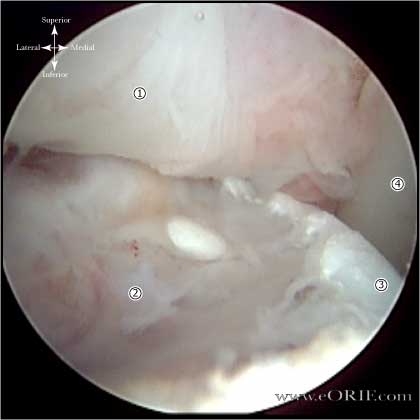
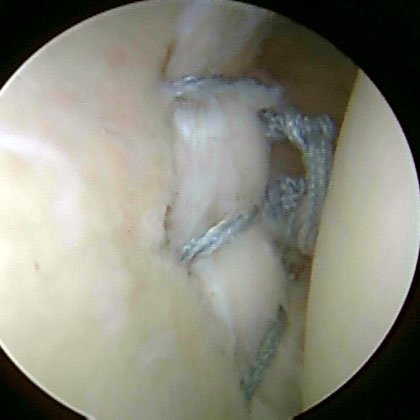
- Bankart lesion = avulsion of the anteroinferior capsulolabrum.
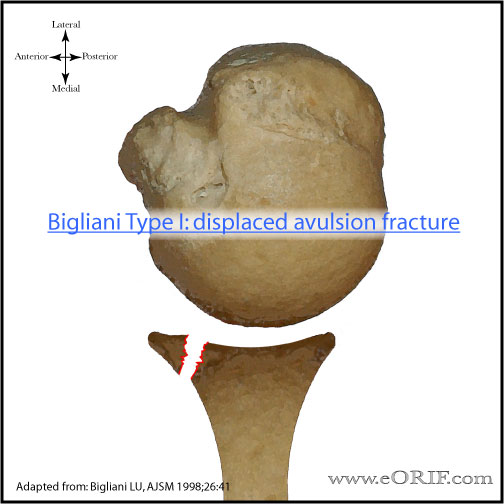
- Bony Bankart = fracture of the anteroinferior glenoid.
- Occurs in 97% of first time acute traumatic dislocations in young patients. (Taylor DC, AJSM 1997;25:306).
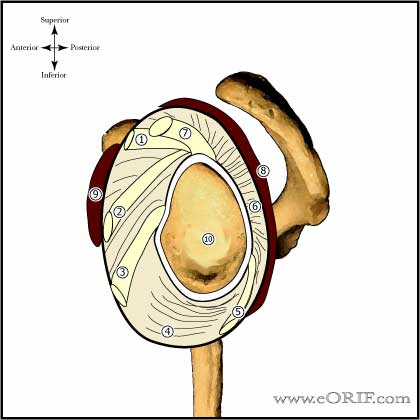
Bankart Anatomy
- Labral functions: origin of many capsuloligamentous structures, increases the depth of the glenoid socket, facilitates the cavity-compression mechanism.
- Blood supply: the labrum receives its blood supply from the suprascapular artery, circumflex scapular branch of the subscapular artery, and the posterior circumflex humeral artery.
- Anterior band of the IGHL is the primary restraint to anterior translation at 90° abduction.
- Buford complex is a normal labral variation.
- Perthes lesion = nondisplaced tear of the anteroinferior labrum held in position by an intact medial scapular periosteum.
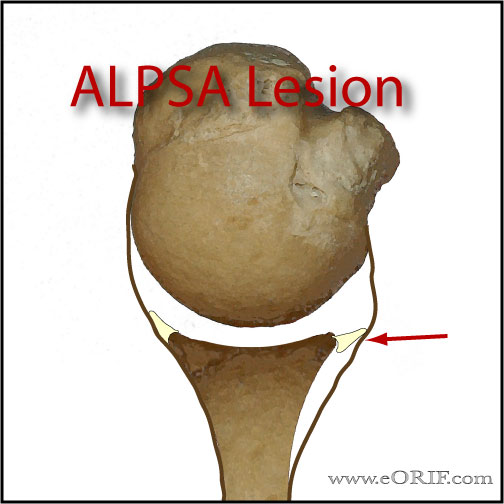
- APLSA lesion = anterior labroligamentous periosteal sleeve avulsion, similar to Perthes lesion except labrum is displaced. (Neviaser TJ, Arthroscopy 1993;9:17).
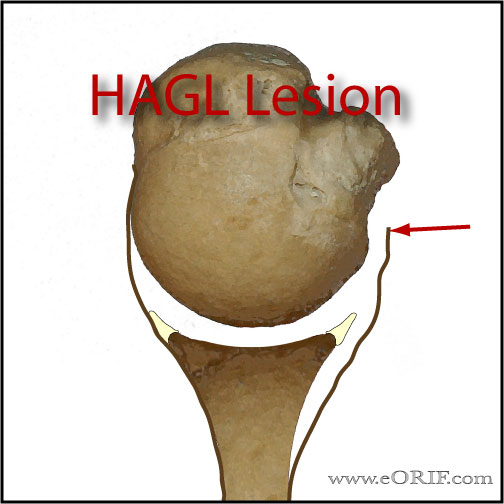
- HAGL lesion = humeral avulsion of the glenohumeral ligaments.
- See also: Shoulder Anatomy
Bankart Clinical Evaluation
- Occurs following traumatic dislocation. May have clicking or popping with shoulder motion.
- Apprehension Test: examiner applies anteriorly directed force to the humeral head with the shoulder in abduction and external rotation. Positive result is the patient felling that the shoulder is going to dislocate.
- Relocation Test t: posteriorly directed force is applied to the humeral head with patient in abduction and external rotation (Apprhension Test position). Positive result is relief of the feeling of impending dislocation.
- Load and shift:
- Sulcus sign : distraction force is applied to the arm with the patient seated with are at the side. The magnitude of displaced and any apprehension sensations are compared to the contralateral limb. Any abnormalities indicated inferior instability.
- Farber JBJS 2006;88A:
- Evaluate axillary nerve function
Bankart Xray / Diagnositc Tests
- A/P and Lateral view in the plane of the scapula, and axillary view. Generally normal.
- West Point view: patient prone with arm in 90° abduction and neutral rotation. Xray beam is directed 25° posterior to the horizontal plane and 25° medial to the vertical plane. Useful for evaluating the anterior glenoid rim / bony bankart lesions.
- Hill-Sachs lesion: impression fracture of the posterosuperior aspect of the humeral head, produced by contact with the anteroinferior glenoid when dislocated. Hill-Sachs lesion is demonstrated on plain AP radiograph in internal rotation.
- CT scan is best to evaluate bony anatomy and should be considered for the recurrent dislocator suspected of having a large Hill-Sachs or bony Bankart lesion.
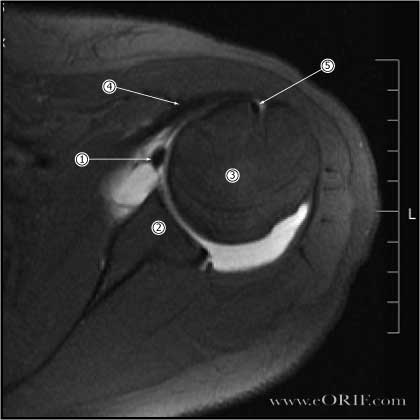
- MRI arthrogram (gadolinium): the anterior and posterior labrum are best seen on axial images and appear as dark triangular structures. Bankart lesions appear as a loss of the normal triangular shape or contrast material may extend between the labrum and glenoid( acute injuries.) Chronic injuries may scar down to the glenoid and be difficult to see by MRI.
Bankart Classification / Treatment
- Consider primary Anterior instability repair for hightly athletic young (<25y/o) patients with MRI confirmed Bankart lesions.
- Bony Bankart Lesion:
-If >25% of the glenoid is involved in a bony-Bankart lesion (anterior rim fracture) the joint will be unstable without ORIF of the bony lesion, or bone grafting the defect. (Bigliani LU, AJSM 1998;26:41)
-Glenoid bone loss (inverted pear glenoid) can be assessed arthroscopically. A 25% reduction in the length from the anterior glenoid to the bare spot in the center of the glenoid compared to the distance from the posterior rim to the bare spot indicates glenoid deficiency and the need for ORIF of the bony lesion, or bone grafting the defect. (Burkhart SS, Arthroscopy 2002;18:488)
-Arthroscopic repair techniques: (Sugaya H, JBJS 2006;88Am:159), (Millett PJ, Arthroscopy 2008),
-Chronic Anterior Instability with Glenoid deficiency: Glenoid deficiency greater than 25% generally requires treatment (bone grafting vs coracoid transfer). Treatment options = Latarjet procedure (Allain J, JBJS 1998;80:841), (Burkart S, AJSM), Tricortical iliac crest great (Warner JJ, AJSM 2006:34:205), Open anterior soft tissue stabilization [large defects loose @7ºER] (Pagnani M, JBJS 2008;36A:1805).
-(Lynch JR, JSES 2009;18:317)
- Engaging Hill-Sachs lesions: consider grafting defect arthrscopically using synthetic bone plugs (Smith& Nephew), or Arthroscopic Hill-Sachs remplissage with arthroscopic posterior capsulodesis and infraspinatus tenodesis. (AAOSNow June2007).
Bankart Associated Injuries / Differential Diagnosis
- Hill-Sachs lesion: impression fracture ot the humeral articular surface caused by translation of the humeral head over the glenoid rim. Found in @85% of anterior dislocations. If >25% of the articular surface is involved allograft or autograft bone graft to repair the defect is indicated
- SLAP Tear 840.7
- Rotator Cuff Tear (RTC) 727.61
- Anterior-Inferior Glenohumeral Instability 718.31
- HAGL lesion
- ALPSA: anterior labroligamentous periosteal sleeve avulsion; medialized Bankart with medial displacement of the torn anterior labrum.
- Perthes lesion: nondisplaced labral tear
- GLAD lesion: glenolabral articular disruption: nondisplaced anterior labral tear associated with articular cartilage injury.
Bankart Complications
- Recurrent instability, Hardware failure, Anchor pull-out, Infection, Stiffness, CRPS, Nerve or vascular injury, Chondrolysis, Hematoma, Chondral Injury, inability to return to sport, incomplete relief of pain, and Arthritis
- Recurrent instability / failure
- Hardware failure / Anchor pull-out
- Infection
- Stiffness
- CRPS
- Nerve injury: Axillary nerve, Brachial plexus
- Fluid Extravasation:
- Chondrolysis: though to be related to heat from electo cautery or radiofrequency probes used during capsular release or capsular shrinkage.
- Hematoma
- Chondral Injury / arthritis
Bankart Follow-up Care
- Post-Op:Shoulder immobilizer. Begin pendelum ROM, elbow/wrist/hand exercises immediately.
- 7-10 Days: continue shoulder immobilizer for 4-6weeks. Start Physical therapy, active assist and active ROM; No external rotation past 40 degrees for 6 weeks.
- 6 Weeks: discontinue shoulder immobilizer. Progress with strengthening exercises.
- 3 Months: Progess with ROM and strengthening, start sport specific training.
- 6 Months: Return to sport if patient has full ROM, near full strength and no apprehension.
- Anterior-Inferior Instability Rehab Protocol.
- Shoulder Outcome Measures
- Outcomes: 90% excellent or good results, 10% recurrent instability . Average ASES score = 92 of 100 points. Patient satisfaction = 8.9 on a 10-point visual analog scale. (Carreira DS, AJSM 2006;34:771). 11% recurrence for collision/contact athletes (Mazzoca AD, AJSM 2005;33:52).
Bankart Review References
|











