|

|
synonyms:medial clavicle fracture, sternal clavicle fracture, fracture of sternal end of clavicle
Medial Clavicle Fracture ICD-10
A - Initial encounter for closed fracture
B - initial encounter for open fracture
D - subsequent encounter for fracture with routine healing
G - subsequent encounter for fracture with delayed healing
K - subsequent encounter for fracture with nonunion
P - subsequent encounter for fracture with malunion
S - sequela
Medial Clavicle Fracture ICD-9
Medial Clavicle Fracture Etiology / Epidemiology / Natural History
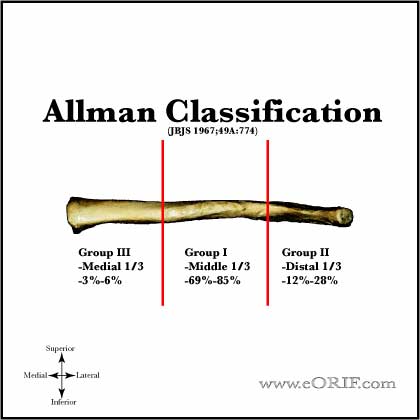
- medial 1/3=3%-6% of clavicle fractures.
- Generally associated with multisystem trauma; 20% mortality second to associated trauma; generally non-operative treatment (Throckmorton T, JSES 2007;16:49).
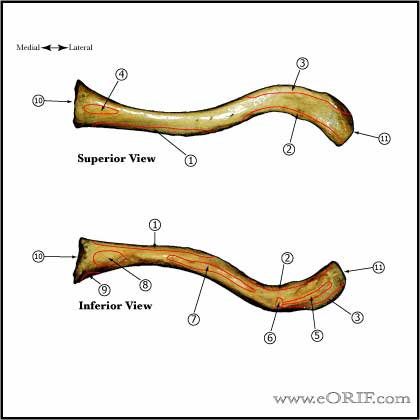
Medial Clavicle Fracture Anatomy
- First bone to ossify, 5th gestational week
- Only long bone to ossify be intramembranous ossification
- Medial physis=80% of longitudinal growth. Last physis to close usually 18-25y/o.
- Both acromial and sternal physes can remain open into 3rd decade of life
- Middle 1/3 fractures typically heal with the lateral shaft fragment displaced posterior to the medial shaft fragment / anterior-posterior angulation. (Edleson JG, JSES 2003;12:173).
- See also Shoulder Anatomy.
Medial Clavicle Fracture Clinical Evaluation
- Associated with dysphagia and shortness of breath; airway management is paramount followed by great vessel evaluation.
- Pain over clavicle, crepitus and motion at fracture site. Often obvious deformity.
- Evaluate skin over fracture site for tenting, inpending skin compromise
- Ptosis of affected shoulder.
- NV exam of upper extremity indicated.
- Auscultate chest to rule out associated pneumothorax.
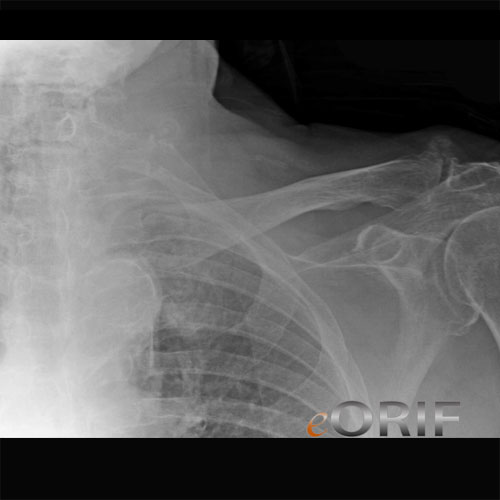
Medial Clavicle Fracture Xray / Diagnositc Tests
- A/P view of clavicle and 30° cephalic tilt view of clavicle.
- Apical oblique (Grashe with 20 cephalad)
- Abduction Lordotic (after ORIF)
- Serendipity view (helps with A/P displacement)
- Axillary
- Zanca 15 degree apical oblique (AC joint)
- Consider chest xray (including both clavicles) if there is significant deformity (shortening) or if concerned for pneumothorax or rib fx's.
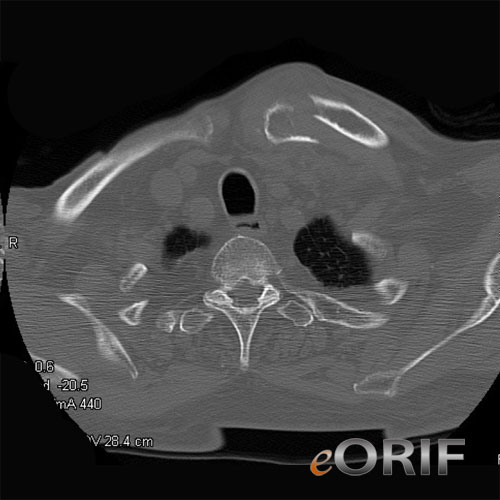
- CT with 3-D reconstruction is helpful for segmental fractures or for medial clavicle fractures which may be missed on Chest xrays.
Medial Clavicle Fracture Classification / Treatment
- Allman Classification (Allman FL, JBJS 49A;774:1967).
- Posteriorly displaced: closed reduction performed in OR with patient’s chest prepped and draped and CT surgeon on standby. Type and crossed blood available. Place folded towels/sandbag between scapulas. Pt supine on table. Apply traction to abducted arm in line with clavicle. Then slowly move arm into mild extension while gently pulling medial clavicle anteriorly. May consider using towel clip to aid in reduction. Closed reduction is typically difficult to maintain if >48hours since injury. If closed reduction is unsuccessful proceed with open reduction with suture fixation of the fracture to the rhomboid (costoclavicular ligament) with sternoclavicular joint stabilization and/or autologous graft reconstruciton of the SC joint. See SC joint reconstruction.
- Posterior physeal injury: closed reduction followed by sling and swathe. Consider open reduction if unable to reduce closed.
- Anterior physeal injury: symptomatic treatement without reduction. Physis will remodel with little to no fuctional limitations.
- Anteriorly displaced: sling and swathe +/- closed reduction depending on amount of displacement.
- Nonunion: consider two-stage reconstruction. Stage 1 = ORIF medial clavicle with bone grafting and mid-clavicle osteotomy. Stage 2 = medail hardware removal and ORIF mid-clavicle osteotomy. (Al-Yassari G, JSES 2009).
- Chronic injuries are unlikely to be reduced closed due to soft tissue interposition/scar
- Never transfix SC joint with wires/pins as HW failure +/- pin migration into chest is the general rule with hardware in the SC joint due to tremendous lever arm on SC joint.
- Displaced medial 1/3 clavicle fractures are at increased risk of cosmetic deformity.
- See also SC Reconstruction Technique.
- ORIF Medial Clavicle fracture (Low AK, JSES 2008;17:751).
Medial Clavicle Fracture Associated Injuries / Differential Diagnosis
Medial Clavicle Fracture Complications
- Nonunion
- Malunion
- Infection
- Neurovascular Injury
- Pneumothorax
- Laceration of superior vena cava, pulmonary artery
- Brachial Plexus Palsy
- Rupture of the aorta or esophagus
- Shortness of breath
- Hoarseness
- Difficulty swallowing
- Thoracic Outlet Syndrome
Medial Clavicle Fracture Follow-up Care
- Post-op: sling for comfort, no overhead motion. Immediate pendelum ROM exercises.
- 10-14 Days: Wound check, sutures removed. Start PT for gentle ROM exercises. No resistive exercises/activities. Sling as needed for comfort.
- 6 weeks: Xrays, if union is evident begin strengthening and resistive exercises. No contant athletics.
- 3 months: Repeat xrays. If pt is painfree and union is obvious pt may return to sport. If no signs of union, consider bone stimulator, see Nonunion.
Medial Clavicle Fracture Review References
- Rockwood, Green, and Wilkins' Fractures: 7th ed.
- Orthopaedic Knowledge Update: Shoulder and Elbow, No. 3, 2008
- Cofield, Springer; Revision and Complex Shoulder Arthroplasty, 2008
- Warner, Iannoti, Flatow; Complex and Revision Problems in Shoulder Surgery, 2005
- Wirth MA, JAAOS, 1996;4:268
|






