|
|
synonyms: radiocapitellar dislocation, elbow dislocation, radiohumeral dislocation, ulnohumeral dislocation
Elbow Dislocation ICD-10
A- initial encounter
D- subsequent encounter
S- sequela
Elbow Dislocation ICD-9
- 832.0_ = closed elbow dislocation; 832.1_ = open elbow dislocation
- 832._0 (dislocation of elbow unspecified)
- 832._1 (anterior dislocation of elbow)
- 832._2 (posterior dislocation of elbow)
- 832._3 (medial dislocation of elbow)
- 832._4 (lateral dislocation of elbow)
- 832._9 (dislocation of elbow other)
Elbow Dislocation Etiology / Epidemiology / Natural History
- 90% posterior or posterlateral dislocations.
- Second most common dislocation of the upper extremity.
- Annual incidence = 5.21 / 100,000 persons. (Stoneback JW, JBJS;2012:94A:240)
- Adolescent males are at highest risk. Nearly half of elbow dislocations occur in sports. Males are at highest risk in football. Females are at highest risk in gymnastics and skating. (Stoneback JW, JBJS;2012:94A:240)
- 75% result from falls on outstretched arms. Generally combined supination, axial compression and valgus forces. (O'Driscoll SW, CORR 1992;280:194).
- Most common residual effect is loss of terminal extension (@15°).
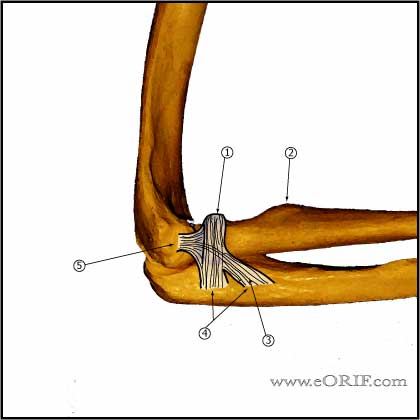
Elbow Dislocation Anatomy
- Primary constraints=ulnohumeral articulation(coronoid), medial collateral ligament(MCL), lateral collateral ligament(LCL) (King GJ, JSES 2;165:1993).
- Secondary constraints=radial head, common flexor and extensor origins, capsule. (Morrey BF, CORR 1991;265:187).
- Dynamic constaints=mucles which cross the elbow, mainly the triceps, anconeus and brachialis.
- Anterior band of medial collateral ligament is the primary constraint to valgus instability.
- LCL(ulnar part) is primary constraint to posterolateral rotatory instability
- Pathoanatomy of dislocation is a circle of bone/soft tissue disruption starting laterally and progressing medially. Stage I=ulnar band of LCL, Stage II=ant/post capsule, Stage III=MCL disrupted, anterior band of MCL is the last to disrupt.
- Most dislocations have disruptions of both the MCL and LCL.
- Posterior elbow dislocations: posterolateral rotatory mechanism; hand is fixed and the body creates a valgus and external rotation moment on the elbow initially tearing of the lateral collateral ligament, then the anterior and posterior joint capsules and finally can tear the ulnar collateral ligament.
- Lateral collateral ligament tear is most commonly an avulsion from the distal humerus (other areas of injury: midsubstance tears, proximal avulsions, distal bony avulsion) (McKee MD, JSES 2003;12:391).
- See also Elbow Anatomy.
Elbow Dislocation Clinical Evaluation
- Generally present with obvious deformity, pain and swelling.
- Document NV exam before and after reduction.
- Lateral pivot shift test=for posterolateral rotatory instability- pt supine, arm overhead. Supination-valgus moment applied during flexion, elbow subluxates usually at @40degrees, additional flexion causes reduction/clunk. Should create apprehension.
- Valgus and varus stress, both in extension and 30 degrees flexion.
- Valgus stress testing performed in full pronation to eliminated posterolateral rotatory instability.
- Document wrist evaluation.
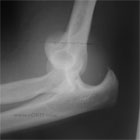
Elbow Dislocation Xray / Diagnositc Tests
- A/P and lateral elbow films demostrates dislocation and associated fractures.
- Evaluate for coronoid fracture: a small flake coronoid fx is indicative of a dislocation/subluxation in which trochlea knocked chip off. If it is larger than 2mm it likely represents varus-posteromedial rotatory instability and has strong propensity for posttraumatic arthritis. (OKU Shoulder and Elbow 2nd ed)
- Consider stress films.
Elbow Dislocation Classification / Treatment
- Reduction maneuver: longitudinal traction with the forearm in supination and gentle guiding of the olecranon forward into a reduced postion.
- Splinting: most stable position following reduction for posterolateral dislocation is elbow flexed and pronated. Radial head is most stable in pronation.
- Simple elbow dislocation = no associated fracture. For elbow dislocations with an osseous component see respective fracture classification and treatment.
- Stages of instability (O'Driscoll, Jupiter, King, Hotchkiss, Morrey,ICL JBJS 82A:724, 2000). Stages can be determined by on EUA or after intraarticular local anesthetic injection with fluoroscopy.
| Stage |
Injured structures |
Clinical Findings after reduction |
Treatment |
| 1 |
ulnar band of LCL disruption |
+lateral pivot shift test, but elbow is stable though ROM. |
Immediate ROM in hinged brace with forearm in neutral rotation. |
| 2 |
coronoid perched on trochlea |
Elbow stable, but may have ulnohumeral gapping near extension. |
Immediate ROM in hinged brace in full pronation for 2 weeks followed by neutral ROM in neutral rotation for 2 wks. |
| 3a |
LCL and posterior band of MCL torn. Anterior band of MCL intact, |
Stable to valgus after reduction, stable in pronation, but ulnohumeral gapping noted in supination near extention. |
Immediate ROM in hinged brace in full pronation for 2 weeks followed by neutral ROM in neutral rotation for 2 wks. |
| 3b |
LCL and entire MCL disrupted, |
Unstable to varus, valgus and posterolateral rotation. Ulnohumeral gapping in supination and pronation near extention. |
If stable at 30° flexion, block extension at 30°-130° and gradually extend; if unstable at 30° surgical repair indicated |
| 3c |
Distal humerus stripped of all soft tissues. |
Grossly unstable even in cast, reduction maintained only with flexion >90degrees. |
Surgical repair indicated |
- Acute=posterolateral rotatory(most common) vs valgus(MCL tear and usually radial head fx) vs varus posteromedial rotatory
- Varus posteromedial rotatory dislocation-occurs during axial loading of elbow in flexion=anteromedial Coronoid Fracture and avulsion of LCL.
- Consider volar forearm fasciotomy if reduction was delayed.
Elbow Dislocation Associated Injuries / Differential Diagnosis
Elbow Dislocation Complications
- Most common complication is elbow stiffness/flexion contracture. When the acute pain has subsided in 5 to 7 days, the patient must begin early active motion exercises. There may be some minor loss of motion, and pts should be apprised of this prior to the reduction. 15% of pts lose >30 degrees of flexion. (Mehlhoff TL, JNJS 70A;244:1988)
- Heterotopic Ossification
- Nerve injuries (rare)
- Redislocation / instability(rare)
- Overall @60% have residual symptoms, mainly loss of extension.
Elbow Dislocation Follow-up Care
- Dependent of Stage (see Classification), and any associated injuries.
- Generally immediate ROM in hinged brace. Consider full pronation for 2 weeks followed by neutral rotation for 2 weeks depending on severity in injury.
- Early active motion is paramont to decrease extension loss. There may be some minor loss of motion, 15% of pts lose > 30 of flexion. (Mehihoff TL, JBJS 1988;70A:244).
- Consider Heterotopic Ossificationprophylaxis.
- See also Elbow Outcome Measures.
Elbow Dislocation Review References
- Rockwood and Green's Fractures in Adults: 2009
- Orthopaedic Knowledge Update: Shoulder and Elbow, No. 3
- Cohen MS, JAAOS 1998;6:15
- Tan V, JAAOS 2005;13:503
- Deland JT, Garg A, Walker PS: Biomechanical basis for elbow hinge-distractor design. Clin Orthop Relat Res 1987;:303-312.
- London JT: Kinematics of the elbow. J Bone Joint Surg Am 1981;63:529-535.
- Madey SM, Bottlang M, Steyers CM, Marsh JL, Brown TD: Hinged external fixation of the elbow: Optimal axis alignment to minimize motion resistance. J Orthop Trauma 2000;14:41-47.
- McKee MD, Bowden SH, King GJ, : Management of recurrent, complex instability of the elbow with a hinged external fixator. J Bone Joint Surg Br 1998;80:1031-1036
- Cobb TK, Morrey BF: Use of distraction arthroplasty in unstable fracture dislocations of the elbow. Clin Orthop Relat Res 1995;:201-210.
- O’Driscoll SW, Jupiter JB, King GJ, Hotchkiss RN, Morrey BF: The unstable elbow. Instr Course Lect 2001;50:89-102.
- Jupiter JB, Ring D: Treatment of unreduced elbow dislocations with hinged external fixation. J Bone Joint Surg Am 2002;84:1630-1635.
- Anakwenze OA, Kancherla K, Iyengar J, Ahmad CS, Levine WN. Posterolateral rotatory instability of the elbow. Am J Sports Med 2014;42(2): 485-491.
|



