|
|
synonyms:dorsal wrist ganglion, volar wrist ganglion
Ganglion ICD-10
Ganglion ICD-9
- 727.41 (Ganglion of joint)
Ganglion Etiology / Epidemiology / Natural History
- Most common soft tissue tumor of hand, 50-70% of masses.
- Soft mucin-filled cyst usually attached to underlying joint capsule, tendon, or tendon sheath
- Women>men, usually second-fourth decade
- May cause pain, weakness. Antecedent trauma in 10% of cases, repeated minor trauma, no correlation with occupation, malignancy never reported
- Intraosseous cysts are occasionally present
- Etiology and pathogenesis unknown
- Contents: clear, viscous mucin containing glucosamine, albumin, globulin, and hyaluronic acid (Soren A, CORR 1966;48:173).
Ganglion Anatomy
- 70% of Dorsal wrist ganglion are from scapholunate ligament
- 65% of Volar wrist ganglions arise form radioscaphoid joint near the scapholunate interval, 34% from scaphotrapezial joint, 1% trapeziometacarpal joint.
- Extensor digitorum brevis manus muscle belly: origin=proximal portion of radiocarpal ligament near the lunate. Incidence =1.1% – 3%. Usually presents as fusiform mass over dorsum of hand between IF and MF. Muscle may become hypertrophied with increased activity and is most noticeable with active finger/wrist extension against resistance, which constricts muscle against extensor retinaculum and causes pain. RX=splinting, NSAIDS, excision if non-op fails.
Ganglion Clinical Evaluation
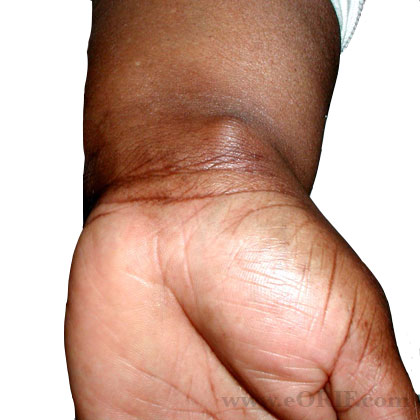
- Compressible, transilluminating, slightly mobile mass; without skin changes
- Wrist extension may elicit pain at the sight
- General normal ROM: flexion=65 (10 functional); extension=55 (35 functional);radial deviation=15 (10 functional); ulnar deviation=35 (15 functional)
Ganglion Xray / Diagnositc Tests
- P/A, lateral and oblique xrays of the wrist are indicated to rule out other causes of wrist pain.
- Occult ganglion dx with MRI; not palpable, but may be quite painful.
Ganglion Classification / Treatment
- Observation up to 50% may resolve with long-term f/u
- Closed rupture=22-60% recurrence
- Cyst puncture & aspiration +/- celestone have limited success: 20-50% recurrence, results may be improved with repeated aspirations and splinting for 3 weeks. Aspiration of volar ganglion risks the radial artery with potential iatrogentic false aneurysm.
- Excision has <10% recurrence rate (dorsal wrist ganglions).
Ganglion Dorsal Ganglion Technique
- CPT: 25111(excision of wrist ganglion, dorsal or volar), 25112(excision recurrent ganglion)
- Supine, arm board, +/-antibiotics, turniquet, 3.5x loupe magnification
- Transvers incision along Langer’s lines
- Skin hooks for retraction, iris/tenotomy scissors
- Mobilze circumferentially, retract extensor tendons(usually 4thcompartment)
- Identify pedicle, dissect to origin(usually scapholunate ligament)
- Excise portion of dorsal wrist capsule and small portion of scapholunate ligament with pedicle.
- Irrigate wound
- Sub-q closure, skin closure
- 5cc 5% bupivicaine for post-op pain
- Dorsal/palmar splint
Ganglion Volar Ganglion Technique
- CPT: 25111(excision of wrist ganglion, dorsal or volar), 25112(excision recurrent ganglion)
- 65% arise form radioscaphoid joint near scapholunate interval, 34% from scaphotrapezial joint, 1% trapeziometacarpal joint.
- Usually located radial to FCR tendon
- Dissection may involve the palm, carpal tunnel, even dorsum of wrist due to extent of cyst
- Protect palmar cutaneous branch of the median nerve and terminal branches of lateral antebrachial cutaneous nerve.
- Follow ganglion down to its origin and excise with small portion of capsule.
- 30% chance of recurrence.
Ganglion Associated Injuries / Differential Diagnosis
- Ganglion of tendon sheath
- Giant cell tumor of tendon sheath
- tenosynovitis, infection
- DISI deformity with prominent proximal pole of scaphoid
- VISI with lunate prominence
- Osteophyte
- Carpometacarpal boss
- Venous aneurysm
- Lipoma
- PIN neuroma
- Hamartoma
- Sarcoma
Ganglion Complications
- Cosmesis(scar)
- Infection
- Nerve injury
- Decreased motion
- Instability
- Complex Regional Pain Syndrome
- We discussed the risks of ganglion excision including but not limited to: incomplete relief of pain, incomplete return of function, cosmesis (scar), infection, nerve or vascular injury, stiffness, wrist instability, CRPS and the risks of anesthesia including heart attack, stroke and death.
Ganglion Follow-up Care
- Elevation x 1wk
- 5-7 day post-op visit
- Immobize wrist with splint 30degrees extension for dorsal ganglion, neutral for palmar ganglion; for 2-3 wks.
- After 2-3 wks begin progressive active ROM exercises.
Ganglion Review References
- Thornburg LE, JAAOS 1999;7:231
- °
|



