|

|
synonyms: massive rotator cuff tear, massive RTC tear, massive RC tear, RTC rupture
Massive RTC Tear ICD-10
- M75.120: Complete rotator cuff tear or rupture of unspecified shoulder, not specified as traumatic
Massive RTC Tear ICD-9
- 727.61 non-traumatic complete rupture of rotator cuff),
- 726.10 (disorder shoulder tendon cuff)
- 840.3 (disorder infraspinatus tendon)
Massive RTC Tear Etiology / Epidemiology / Natural History
- Definition: RTC tear with: maximum diameter >5cm or disinsertion into the tuberosites of at least two complete tendons
- Posterior rotator interval(interval between supraspinatus and infraspinatus) is found by identifying scapular spine.
- Linked to calcium phosphate and calcium hydroxyapatiite crystals
- Generally 6th-8th
- MUST ENSURE CORACOACROMIAL ARCH IS PRESERVED
Massive RTC Tear Anatomy
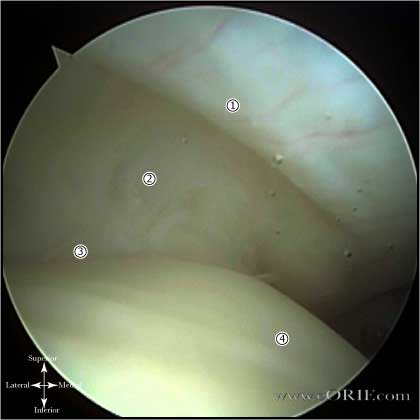
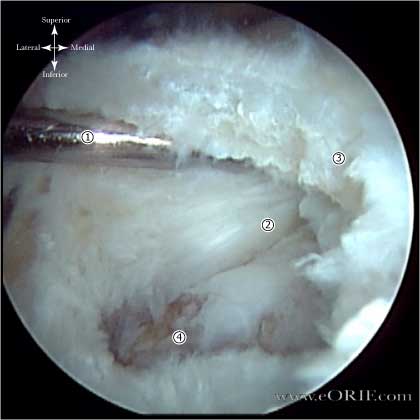
- Rotator cable-rotator crescent complex: an arching, cable-like thickening surrounding a thinner crescent of tissue that inserts into the greater tuberosity of the humerus seen when the RTC is viewed intra-articularly. The rotator cable is 2.59 times the thickness of the rotator crescent that it surrounds and functions to stress-shield the rotator crescent. (Burkhart SS, Arthroscopy 1993; 9: 611-616)
- Scapular spine: resembles the keel of a boat when viewed arthroscopically after excision of its surrounding subacromial fibroadipose tissue, and serves as a marker between the supraspinatus and infraspinatus
- Suprascapular nerve: At risk during the posterior interval slide. Curves tightly around the base of the scapular spine at its junction with the posterior glenoid neck, enveloped within a fat pad. The average distance from the origin of the long tendon of the biceps to the motor branches of the supraspinatus is 2 cm. The average distance from the posterior rim of the glenoid to the motor branches of the infraspinatus muscle is 2cm. (Warner JJP,JBJS 1992; 74Am: 36-45)
- Coracoacromial Ligament: Must not be disrupted in patients with RTC tears.
- Long head of Biceps Tendon:
- See also Shoulder anatomy.
Massive RTC Tear Clinical Evaluation
- Supraspinatus and infraspinatus atrophy. Patients may have associated suprascapular neuropathy (Mallon WJ, JSES 2006;15:395).
- Passive and active ROM discrepancy.
- Lag sign: tests posteriosuperior RTC. Arm is placed in maximal ER. Pts with a massive RTC tear will be unable to maintain the arm in the position and the arm will swing toward neutral rotation.
- Hornblower's Sign: patient is unable to ER the arm to 90 degrees with the arm in abduction. Indicates massive tear usually including the teres minor.
- Subscapularis is tested with lift-off test and abdominal compresison test.
Massive RTC Tear Xray / Diagnositc Tests
- AP, scapular lateral and axillary views. . Evaluate for acromial spur, greater tuberosity sclerosis/cysts, loss of acromiohumeral interval.
- Supraspinatus "outlet" view lateral radiographic view of the scapula and acromion, with a 20-degree caudal tilt. Intended to identify any bone projecting downward into the supraspinatus outlet.
- Acromiohumeral interval measured on true AP view in neutral rotation <7mm = superior subluxation of humeral head. Indicates chronic long standing massive tear and is associated with failures of direct repair.
- Note proximal migration of humeral head, sclerosis of the undersurface of the acromion and superior humeral head, acetabularization of the undersurface of the acromion, degenerative changes of the GH joint.
- Evaluate for subacromial arthritis
- Goutallier Classification of Muscle Atrophy (Goutallier D, CORR 1994;304:78).
-Stage 0=completely normal muscle.
-Stage 1=muscle contains some fatty streaks.
-Stage 2=fatty infiltration is important, but there is still more muscle than fat.
-Stage 3=there is as much fat as muscle.
-Stage 4=more fat than muscle is present.
-Degeneration is grade at the tip of the coracoid process and at the inferior margin of the glenoid and the values are averaged to determine the stage.
- GFDI(global fatty degeneration index) = mean fatty infiltration score of subscap, supraspinatus and infraspinatus. <0.5 = retear rate <25%. GFDI>2 = 100% retear rate.
- Hamada Classification of Arthritis in chronic rotator cuff tears (Hamada K, CORR 1990;254:92).
Stage 1: Acromiohumeral interval greater than 6 mm.
Stage 2: Acromiohumeral interval less than 7 mm.
Stage 3: Acromiohumeral interval less than 7 mm with acetabulization of acromion.
Stage 4a: Acromiohumeral interval less than 7 mm with glenohumeral arthritis without acetabulization.
Stage 4b: Acromiohumeral interval less than 7 mm with acetabulization and glenohumeral arthritis.
Stage 5: Acromiohumeral interval less than 7 mm with osteonecrosis of humeral head.
Massive RTC Tear Classification / Treatment
- Low functional demands, asymptomatic. If patient has a tolerable pain level and is able to do ADL’s non-operative treatment with below elbow level physical therapy as needed is indicated
- Low functional demands, severe pain: subacromial injection > scope with biceps tenotomy, acromial smoothing, debridement. 83% patient satisfaction. Be sure to preserve acromion and CA arch. Goals of surgery are pain relief not functional recovery. (Walch G, JSES 2005;14:238).
- High functional demands, acromial-humeral interval >7mm: Rotator Cuff Repair
- High functional demands, acromial-humeral interval <7mm: consider partial repair +/- tendon transfers vs fusion vs hemiarthroplasty vs reverse TSA. Goals of surgery are pain relief not functional recovery.
- Latissmus dorsi transfer results only good if subacapularis intact (Aoki JBJS 1996;78Br:761-766). Works best for patients with lack of ER pre-op.
- Consider Biceps tenotomy if tendon is degenerated and especially if subluxated into joint.
- Hemiarthroplasty (Field, JSES 1997;6:18-23)
- Scope, decompression (Gartsman JBJS 1997;79A:715-721)
- Consider concomittent biceps tenotomy.
- Consider Superior capsular reconstruction: no long term outcomes available. Consider for Hamada Stage 1,2. @70% successful. Use human dermal graft. Very slow gentle rehab.
- Superior Capsular Reconstruction CPT coding: 29999 unlisted code: AAOS recommends comparing to CPT codes 29827 and 29806.
- Consider rotator cuff augmenation. Limited outcome data available. May consider for yourger patients with larger tears.
- Subacromial bio-degradable balloon: not FDA approved in USA. 80% improved pain/Constant scores for @24 months. Improves pain, but not function.
- Lower Trapezius Transfer: requires use of Acilles allgraft (Elhassam B, JSES 2016). Technique.
Massive RTC Tear Muscle Transfers
- Anterosuperior tears(involve subscapularis and supraspinatus): treated with pectoralis major transfer. (Resch H, JBJS 2000;82A:372), (Jost B, JBJS 2003;85A:1944). Biomechanically pec transfer under the conjoined tendon perform better (Konrad GG, JBJS 2007;89A:2477)
- Posterosuperior tears(involve infraspinatus and supraspinatur): treated with latissmus dorsi and or teres major transfer. (Gerber C, CORR 1988;232:51) (Warner JJ, JSES 2001;10:514)
- See Latissmus dorsi transfer technique.
Massive RTC Tear Associated Injuries / Differential Diagnosis
- RTC tear
- Frozen shoulder
- Shoulder instability
- Glenohumeral arthritis
- AC disorders
- Fibromyalgia
- Calcific tendonitis
- Cervical radiculitis
- Viral plexopathy(Parsonage-Turner syndrome)
Massive RTC Tear Complications
- Recurrent tear: high failure rate for repair of tears with Acromiohumeral interval <5mm, marked muscle atrophy and fatty degeneration.
- Hardware failure / Anchor pull-out
- Acromion fx
- Infections
- Stiffness
- CRPS
- Nerve injury: Axillary nerve, Brachial plexus
- Fluid Extravasation:
- Chondrolysis: though to be related to heat from electo cautery or radiofrequency probes used during capsular release or capsular shrinkage.
- Hematoma
- Chondral Injury / arthritis
- Instrument failure
- Deltoid dehiscence (open repair)
- Anterior-superior instability / migration: Do not disrupt acromiohumeral ligament
- Suprascapular neuropathy (Mallon WJ, JSES 2006;15:395)
Massive RTC Tear Follow-up Care
- abduction splint for 6weeks. Abduction of 30 degrees has been shown to substantially reduce tensions on a supraspinatus repair.
- Outomes of arthroscopic repair of massive rotator cuff tear: 94% rate of failure of healing, at two years follow-up. 10 year follow up nearly all with have proximal humeral migration or cuff tear arthropathy. Clinical improvements and pain relief are durable at 10 year follow up despite failure of repair. (Paxton ES, JBJS 2013;95A(7);627)
Massive RTC Tear Review References
- Burkhart SS, A Cowboy's Guide to Advanced Shoulder Arthroscopy, 2006
- Rockwood and Green's Fractures in Adults 6th ed, 2006
- OKU - Shoulder and Elbow 2nd ed, 2002
- Williams GR, Rockwood CA Jr, Bigliani LU, Iannotti JP, Stanwood W, Rotator Cuff Tears: Why do we repair them? JBJS 2004:86A:2764)
- Warner JP, JBJS 2000:82:878
|




