|
|
synonyms: SCFE
Slipped Capital Femoral Epiphysis ICD-10
Slipped Capital Femoral Epiphysis CPT Codes
Slipped Capital Femoral Epiphysis ICD-9
- 820.00(closed unspecified intracapsular) 820.10(open unspecified intracapsular)
- 820.01(closed ephiphseal separation) 820.11 (open ephiphseal separation)
Slipped Capital Femoral Epiphysis Etiology / Epidemiology / Natural History
- Posterior and inferior slippage of proximal femoral epiphysis on metaphysis
- Actually epiphysis is held in acetabulum by ligamentum teres while metaphysis moves upward and outward
- Etiology=multifactorial, occurs during adolescent growth spurt.
- Risk Factors: obese, increased physeal obliquity and increased femoral retroversion, associatation with hypothyroidism, GH deficiency, hypogonadism, renal failure osteodystrophy, previous radiation therapy, African-American decent
- @2/100,000 person; 0.2/100,000 in eastern Japan, 2.13/100,000 in southwestern US, 10.08/100,000 in Northeastern US
- Boys>girls, black>white
- average age girls=12.01, boys=13.5
- 60% of pts are over the 95thpercentile for weight
- 18%-63% bilateral, 82% of second cases occur within 18 months
- Rate of osteonecrosis is nearly 0% following treatment of a stable slip, estimates of the rate after an unstable slip range from 10% to 60%.
Slipped Capital Femoral Epiphysis Anatomy
- Slip occurs through the physeal zone of hypertrophy, gradually progresses until physeal closure
- main blood supply = lateral epiphyseal vessels(branch of medial femoral circumflex, enter posterosuperiorly and anastomose with vessels from ligamentum teres near the junction of the medial and central thirds of the femoral head. Inferior metaphyseal vessels enter anteroinferiorly and anastomose with the previous vessels, but the physis acts as a barrier. (Brodetti)
- Avoid screw placement in posterosuperior quadrant to avoid lateral epiphyseal vessels. Ideal position is central
Slipped Capital Femoral Epiphysis Clinical Evaluation
- Dull, aching, chonic or intermittent hip, groin, thigh or knee pain. Pain may be increased with activity. May present with main complaint of knee pain (Kocher MJ, JPO 1999:19:455).
- ER gait, thigh atrophy
- Loss of IR
- increased ER
- May have leg-length discrepancy.
- obligatory ER with hip flexion
- unstable slip pt usually holds hip flexed and ER
- Whitman's sign--hip flexion past 90 causes hip to externally rorate
Slipped Capital Femoral Epiphysis Xray / Diagnositc Tests
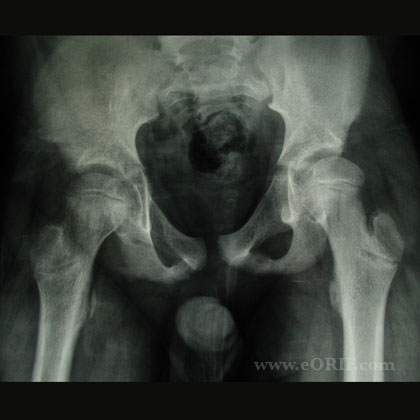
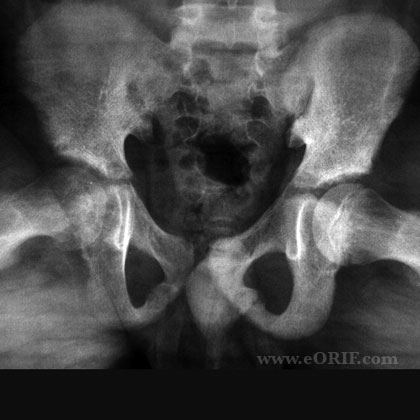
- AP and lateral pelvis films, lateral can be frog-legged or cross table
- Kleins Line--a line drawn along the superior border of the femoral neck on A/P view usually intersects the lateral part of the epiphysis but fails to do so in the presence of SCFE
- Southwick xray classification-based on frog-leg lateral views; value of head-shaft angle of normal side is subtracted from that of the affected side: 0-29=mild;30-60=moderate; >60=severe. For bilateral subtract 12 degrees from head-shaft angle
- Steel's metaphyseal blanch sign-double density at the level of the metaphysis reflecting the posterior cortical lip of the epiphysis as it is beginning to slip posteriorly and is superimposed on the metaphysis. (Steel, JBJS 68-A;920-922, 1986)
- US may be more sensitive at detecting mild slips, bone scan not recommended, MRI CT generally not indicated, MRI can detect AVN earlier than xray(marrow changes)
- In the preslipping, or minimal slip stage the earliest radiographic sign is widening and irregularity of the physis with rarefaction in its juxtaepiphyseal portion. This can be detected in the AP projection in a good quality radiogram. A slip may, however, escape notice in the AP view; it is imperative to take views in the lateral plane also to demonstrate actual slipping, which is always posterior initially. The frog-leg lateral projection is often satisfactory
- Labs: CBC, ESR, CRP consider to eval for infection in DDX.
Slipped Capital Femoral Epiphysis Classification / Treatment
- Loder Classification (Loder RT; JBJS 1993;75A:1134)
- Traditional=pre-slip, acute, chronic, acute-on-chronic (does not predict prognosis)
- Stable=able to walk with or without crutches. -intermittent limp, +/- thigh, knee, groin pain. PE=loss of internal rotation/abduction/flexion, spontaneous external rotation with hip flexion. Possible limb length discrepancy and ER gait. fewer than 10%AVN, 96% satisfactory result. As noted by Howorth, avn does not occur in untreated stable SCFE
- Unstable=unable to walk. . Lies still with LE in flexion, abduction, ER. Analagous to SH-I fx prognosis guarded=AVN up to 50%, 47% satisfactory results
- >95% of SCFE's are stable
- ultrasound classification-stable=metaphyseal remodeling, no effusion. Unstable=effusion, no metaphyseal remodeling.
SCFE Treatment
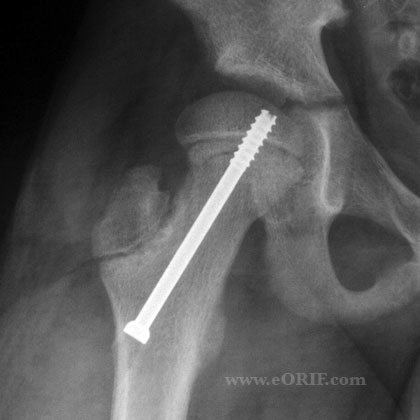
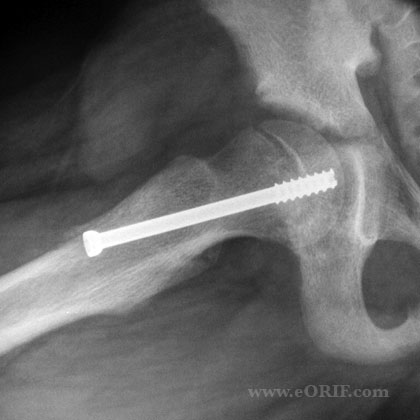
- Stabilization in situ-safest treatment, 95% excellent to good results, 2%AVN
- Correction of deformity at physeal level with stabilization; reduction associated with increased AVN, chrondrolysis
- Modified Dunn procedure (Ziebarth K; Clin Orthop Relat Res. 2009;467(3):704): surgical dislocation, preserves blood supply and allows reduction of epiphysis. 15% broken implants; 26% osteonecrosis; mean slip angle= 6° at follow up (Sankar WN, JBJS 2013;95A:585).
- epiphysiodesis- iliofemoral exposure, window cut in anterior femoral neck and corticocancellous graft driven across physis. +quicker physeal closure, better placement, low risk of protrusion. -42% progression, 6%AVN, 5%chondrolysis, blood loss, longer anesthesia, scar: results some great, some terrible
- Severe SCFE with limitated ROM: proximal femoral osteotomy with stabilization in situ/introchanteric osteotomy with IF. (Diab M, CORR 2004;427:204).
- spica cast immobilization until physis closes, average 12wks, risk of progression(5-10%), chondrolysis(19%), pressure sores bad in obese kids
SCFE Technique
- ASNIS canulated screw set (Howmedica)
- usually supine on fracture table
- must have good views in both A/P and lat plains before starting
- Draws lines on skin in both planes along proper screw insertion planes to determine skin incision.
- Keep in mind the greater the slip, the more anterior your starting point will be. Want screw perpendicular to physis in both planes.
- Avoid multiple entrance holes as this increases risk of fracture.
- Increasing number of screws used has been correlated with increasing number of complications.
- Advance screw until 4-5 threads are across the physis.
- Avoid posterosuperior quadrant pin placement as this risks the lateral epiphseal vessels, ie AVN
- pin protrusion correlated with chondrolysis
Slipped Capital Femoral Epiphysis Associated Injuries / Differential Diagnosis
- Toxic synovitis
- Osteomyelitis
- Septic arthritis
Slipped Capital Femoral Epiphysis Complications
- AVN-increased risk if unstable, postersuperior quadrant pin placement
- Chondrolysis=narrowing of the joint space to at least one-half of that in the contralateral hip in unilateral casea and >3mm in bilateral cases. 5-7%. Increased risk with permanent pin penetration.
Slipped Capital Femoral Epiphysis Follow-up Care
- usually partial weight bearing for 6wks.
- screw can be removed after physis is closed
- long-term results are correlated with initially degree of slippage, Iowa hip scores decrease as degree increases. Residual deformity of the proximal aspect of the femur after in situ treatment leads to development of femoroacetabular impingement, reduced hip motion, and premature osteoarthritis (Sankar WN, JBJS 2013;95A:585)
- Risk of Bilateral SCFE can be assessed by determining bone age. Lower bone age is correleated with increased risk of bilateral SCFE (Loder RT, JPO 2006;26:300).
- Aronson JBJS outcome study
Slipped Capital Femoral Epiphysis Review References
|




