|
|
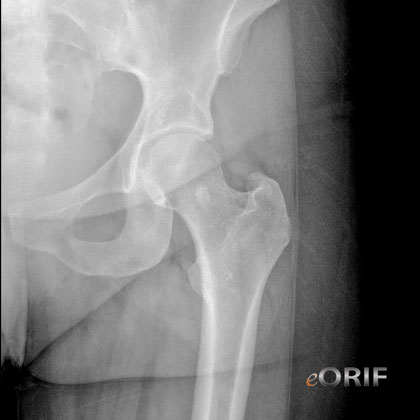
Key Radiographic Findings
1-Cortical destruction, 2-Periostitis, 3-Zone of transition
- Benign:
1-No cortical destruction
2-Benign periostitis: thick wavy, uniform or dense = low-grade chronic irritation
3-Narrow zone of transition; can be traced with a pencil
- Malignant:
1-Cortical destruction
2-Aggressive periostitis: lamellated (onion-skinned), amorphous, sunburst
3- Wide zone of transition; imperceptible
- Permeative lesions (multiple small holes): not easily categorized as benign vs malignant: multiple myeloma, primary lymphoma of bone, Ewing's sarcoma
Benign Skeletal neoplasm fracture risks
-plain radiograph criteria: increased risk of fracture if the defect length is >3.3 cm, the defect width is >2.5 cm or there is more than 50% of the cortex involved as measured on A/P or lateral x-rays.
-CT-based rigidity analysis is more specific (97% specific vs 12% for xray). (Leong NL, JBJS 2010;92:1827)
Metastatic Bone Disease
- "viscious cycle" of lytic bone metastases from TGFb-mediated release of PTHrP stimulating osteoclastic resorption of bone and releasing more TGFb. Consider antiresorptive therapy with zoledronic acid or denosumab.
- Bickels J, JBJS 2009;91A:1503
- Biermann S, JBJS 2009;91A:1518
Syndromes
- Mazabraud Syndrome: fibrous dysplasia and intramuscular myxomas. Rarely can develop osteosarcoma. (Crawford EA, JBJS 2009;91A:955
- Klippel-Trenaunay Syndrome: rare congenital disorder characterized by the triad of cutaneous capillary malformation, varicose veins, and hypertrophy of bone and soft tissue (Kihiczak GG, Int J Dermatol 2006;45:883).
- Morquio Disease (MPS IV): autosommal-recessive defect in the activity of one of two enzymes, N-acetylgalactosamine-6-sulfate (MPS-IVA_ or beta-galactosidase (MPS IVB); results in the accumulation of keratan sulfate and chondroitin-6 sulfate (Montano AM, J Inherit Metab Dis 2007;30:165).
- Fibrodysplasia Ossificans Progressiva: rare; disabling autosomal dominant disorder of joint malformation and progressive heterotopic ossification caused by a recurrent missense point mutation in activin receptor IA (ACVRI / ALK2 / a BMP type I receptor). (Moore R, JBJS 2009;91A:1497).
- McCune-Albright syndrome: polyostotic fibrous dyplasia and endocrine disturbances, especially precocious puberty. Hyperpigmentantion with jagged border("Coast of Maine" border).
Lipoma
- MRI:homogenous with density of subcutaneous fat on all sequences.No enhancement
- Treatment =marginal excision.
Aneurysmal bone cysts
- frequently occur in the first two to three decades of life
- pain and a slow-growing lesion.
- Xray= expansile lesion with septae or striations.
- Treatment = curettage and grafting of the lesion.
Osteomyelitis
- xray = typically shows lucency of bone, periosteal reaction, and a permeative pattern
Giant cell tumor of the tendon sheath
- often arises from the synovial lining of tendon sheaths
- frequently found in the hand and foot. Slow growing but can invade adjacent structures.
- Treatment = excision
Giant cell tumor
- epiphysis of long bone
- xray = radiolucent lesion with a small rim of reactive bone.
Neurilemoma (Schwannoma)
- benign tumor of nerve sheath (Schwann cell) origin
- solitary, well-encapsulated lesion located on the surface of a peripheral nerve.
- Treatment = excision without damaging the underlying nerve
Neurofibroma
- spindle cell tumor arising within a peripheral nerve. Invasive
- Due to its location, it can interfere with distal nerve function
- solitary or multiple
- von Recklinghausen's disease.
- Treatment = resection which requires removal of the affected nerve with resultant distal nerve dysfunction
Enchondroma
- Benign tumor of hyaline cartilage
- most frequently occurs in an intramedullary metaphyseal location.
- Radiologic characteristics: cartilage mineralization pattern (rings, arcs and stippled calcifications); minimal to no endosteal scalloping.
- Follow clinically and radiologically to ensure there is interval change.
- Douis H, Saifuddin A. The imaging of cartilaginous bone tumours. I. Benign lesions. Skeletal Radiol. 2012 Sep;41(10):1195-212.
- Weber KL, O'Conner MI: Benign cartilage tumors. In: Schwartz HS, ed. Orthopaedic Knowledge Update: Musculoskeletal Tumors 2. Rosemont, IL: AAOS; 2007:103-120.
Chondrosarcoma
- Radiologic features: endosteal scalloping, periosteal reaction, cortical destruction, and soft-tissue extension.
Dedifferentiated chondrosarcoma
- Imaging: areas of stippled, chondroid-type calcification and cortical destruction.
- MRI: extraosseous extension that is not seen in a typical low-grade chondrosarcoma.
- Hstology: areas of low and high-grade lobular chondroid material with no osteoid matrix.
Soft-tissue mass
- Subfascial masses which enhance on contrast MRI should be biopsied for definitive diagnosis. Soft-tissue sarcomas can be painless with minimal symptoms.
Fibrous Dyplasia
- "ground glass" appearance
- Parekh SG, Donthineni-Rao R, Ricchetti E, Lackman RD. Fibrous dysplasia. J Am Acad Orthop Surg. 2004 Sep-Oct;12(5):305-13
Desmoid tumor: Desmoid fibromatosis can be associated with adenomatous polyposis coli; consider colonoscopy to screen for colon polyps.
|

