|

|
synonyms: reverse TSA, reverseTSA
Reverse TSA CPT
Reverse TSA Indications
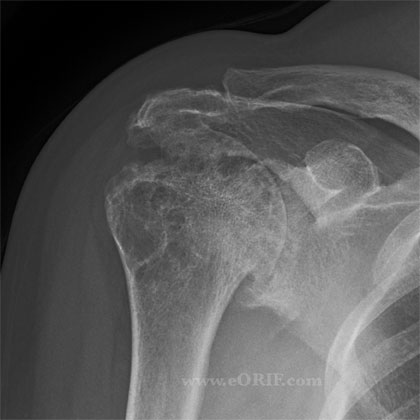
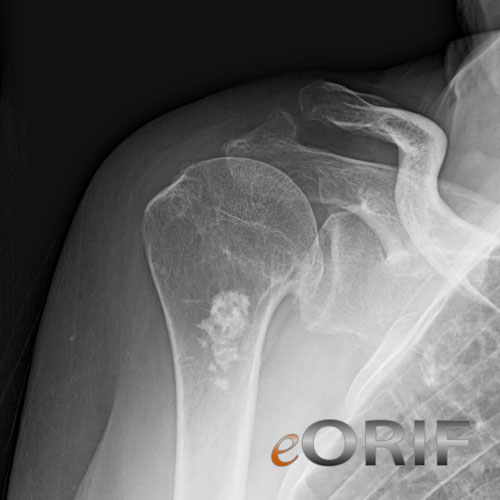
- RTC Arthropathy
- Persistent shoulder pseudo-paralysis due to a massive and irreparable cuff tear
- Acute 3 and 4 part proximal humerus fracture in patients >70yrs old (Bufquin T, JBJS 2007;89Br:516)
- Revision of failed treatment of proximal humerus fractures
- Failed TSA in a cuff-deficient shoulder
- Tumor surgery
- Superior migration of the humeral head
Reverse TSA Contraindications
- Infection / Active sepsis
- Nonfunctioning deltoid / neuromuscular disease
- Axillary nerve palsy
- Insuffient glenoid bone stock
- Young age, high activity level. (Guery J, JBJS 2006;88A:1742).
- Noncompliance
- Medical comorbidities precluding surgery
- Severe osteopenia
- Pregnancy
- Metal allergy
Reverse TSA Alternatives
- Shoulder arthroscopy with debridement and biceps tenotomy
- Hemiarthroplasty: consider for patients with AFE>60°, an intact coracoacromial arch and a desire to maintain rotation.
- Shoulder arthrodesis
- Total Shoulder arthroplasty
- Non-operative management: NSAIDs, PT, steriod injections.
Reverse TSA Pre-op Planning / Special Considerations
- Biomet Comprehensive Reverse TSA
- DJO Global RSP Monoblock reverse TSA
- Zimmer PSI Trabecular metal reverse TSA
- Zimmer Inverse/Reverse TSA
- Tornier Aqualis and Ascend Flex Reverse TSA
- Depuy Delta Xtend reverse TSA
- Most inform patient that reverse TSA will lengthen the arm, and change the contour of the shoulder (not as noticable if Encore prosthesis is used).
- Evaluate MRI for teres minor atrophy. Stage 3-4 fatty infiltration of the teres minor comprises the outcomes for reverse TSA. (Simovitch RW, JBJS 2007;89A:934).
- The arm should be lengthened by @2-3cm (tip of the acromion to the elbow) (Gerber C, JAAOS 2009;17:284).
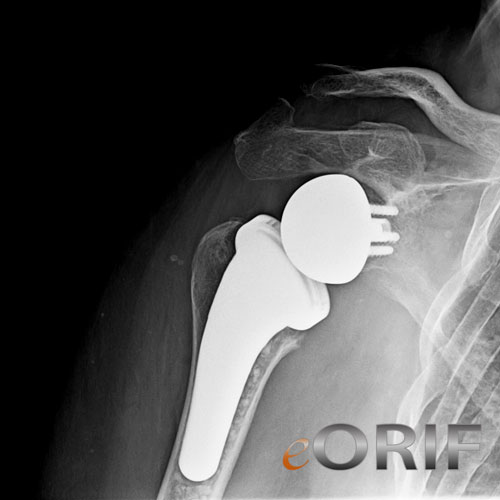
Reverse TSA Technique
- Pre-operative antibiotics, +/- regional block
- Beach chair, ensure unobstructed movement of the shoulder in adduction and hyperextension. All bony prominences well padded.
- General endotracheal anesthesia.
- Examination under anesthesia.
- Prep and drape in standard sterile fashion.
- Extended deltopectoral approach with release of 2/3 of pectoralis major
- Release subdeltoid, subacromial and subcoracoid spaces
- Release subscapularis just medial to long head of biceps
- Dislocate shoulder and resect any osteophytes
- Neck cut at 30 degrees retroversion
- Ensure lateralized humeral entry point, canal reamed and broached to size
- Ream humerus to smallest size, remove medial bone to aid in glenoid exposure
- Capsular release, expose glenoid, considering using k-wires to help define glenoid neck anatomy
- Drill glenoid centering hole in center of inferior 1/3 circle, (length of final center screw is 30mm), ream glenoid (Encore prosthesis).
- Screw in baseplate and fix with 3.5mm peripheral screws
- Place glenosphere
- Trial reduction
- Select humeral component to allow 2mm circumferential cement mantle.
- Place drill holes and sutures in lesser tuberosity for later subscapularis repair.
- Cement final humeral component in place.
- Test stability: dislocation generally occurs anteriorly with the arm in abduction and internal rotation (occurs when getting out of chair or bed). If unstable increase the anterosion of the humerus and ensure glenoid is not anteverted.
- Repair subscapularis throught drill holes.
- Irrigate.
- Closure.
Reverse TSA Complications
- Prevalence: 47% for revision cases, 5% for primary reverse TSA. (Boileau P, JSES 2006;15:527). Complication rate is approximately 3x's that of standard TSA.
- Acromion fracture
- Scapular fracture
- Periprosthetic humeral fracture
- Glenoid fracture
- Infection
- Dislocation / Instability
- Hematoma: most frequent complication in early series.
- Nerve injury: Axillary nerve, Brachial plexus
- Loosening / failure: caused by infection or failure of glenoid ingrowth with eventual metal fatigue and failure (usually around 2 years)
- Polyethylene wear / osteolysis
- Scapular notching (Delta prosthesis) (Simovitch RW, JBJS 2007;89A:588)
- Generally lengthens arm and changes the coutour or the shoulder.
- Metal sensitivity / allergy
- Heterotopic Ossification
- Medical complications: DVT / PE, Myocardial infarction
Reverse TSA Follow-up care
- Post-op: Abduction sling. Elbow, wrist, hand and Pendulum ROM exercises. May move within comfort level right away.
- 7-10 days: continue sling/immobilizer until 3-6 weeks post-op when out and about. Start early passive shoulder ROM( limited to 90 degrees elevation, 0 degrees ER), active elbow, wrist, hand ROM.
- Avoid ER for 6weeks to allow subscapularis to heal.
- Avoid combined abduction and external rotation (risks dislocation).
- 6 Weeks: Active supine ROM started. Discontinue immobilizer, consider using sling in public/crowds. Generally may use arm for daily activities and driving.
- Resistive exercises started at 10-12 weeks
- 3 Months: activity as tolerated. Adjust home exercise program to any patient deficits. May return to golf.
- Radiographic results deteriorate after @6 years, clinical results deteriorate at 6-8 years post-op (Gerber C, JAAOS 2009;17:284)..
Reverse TSA Outcomes
- 68% good/excellent outcomes, 27% satisified, 5% dissatisfied as rated by patients. FE increase from 55° to 105; Abduction from 41° to 102°, ER from 12° to 41°; 17% complication rate, 12% required revision; Encore prosthesis . (Frankle M, JBJS 2005;87A:1697).
- 18% required revision in primary revTSA patiens, 38% revision for secondary surgeries; Depuy Delta III prosthesis. (Werner CM, JBJS 2005;87A:1476).
- 90% satisfied/very satisfied, Constant score pre-op = 24, post-op = 62 (mean 52 month f/u), elevation pre-op = 71º, post-op = 130º. Mole D, Rev Chir Orthop Reparatirce Appar Mot 2007;93(6):37
- Generally improves active elevation, but does not improve active external rotation or internal rotation.
Reverse TSA Review References
- Orthopaedic Knowledge Update: Shoulder and Elbow, No. 3

- Shoulder Arthroplasty
 AAOS Monograph Sanchez-Sotelo editor, 2012 AAOS Monograph Sanchez-Sotelo editor, 2012
- Bigliani LU, Flatow EL, Shoulder Arthroplasty, 2010

- OKU - Shoulder and Elbow 2nd ed, 2002
- Gerber C, JAAOS 2009;17:284
- Gutiérrez S, Levy JC, Frankle MA, Cuff D, Keller TS, Pupello DR, Lee WE 3rd. Evaluation of abduction range of motion and avoidance of inferior scapular impingement in a reverse shoulder model. J Shoulder Elbow Surg. 2008 Jul-Aug;17(4):608-15. Epub 2008 Mar 6.
- Lévigne C, Boileau P, Favard L, Garaud P, Molé D, Sirveaux F, Walch G. Scapular notching in reverse shoulder arthroplasty. J Shoulder Elbow Surg. 2008 Nov-Dec;17(6):925-35. Epub 2008 Jun 16.
- Cheung E, Willis M, Walker M, Clark R, Frankle MA. Complications in reverse total shoulder arthroplasty. J Am Acad Orthop Surg. 2011 Jul;19(7):439-49. Full text
|