|
|
synonyms: wrist scaphoid fracture nonunion, wrist navicular fracture nonunion
Scaphoid Nonunion ICD-10
Scaphoid Nonunion ICD-9
- 733.8 = Nonuion of fracture
Scaphoid Nonunion Etiology / Epidemiology / Natural History
- scaphoid fx that have not healed with 3 months of cast immobiliztion
- scaphoid fx’s that do not show radiographic signs of healing in 6-8wks or those that are diagnosed 6wks after injury are less likely to heal.
- acute fx with collapse, humpback deformity, comminution, displacement >1mm, intrascaphoid angle >45, height-to-length ratio >0.65, poor pt compliance have higher incidence of malunion and nonunion
Scaphoid Nonunion Anatomy
- dorsal scaphoid branch of radial artery supplies 70-80% of scaphoid.(Gelberman J Hand Surg 5A:508, 1980)
Scaphoid Nonunion Clinical Evaluation
- usually asymptomatic early
- wrist pain, loss of motion
- pain in snuffbox is unreliable
- lead to wrist pain, a collapse deformity and progressive arthrosis
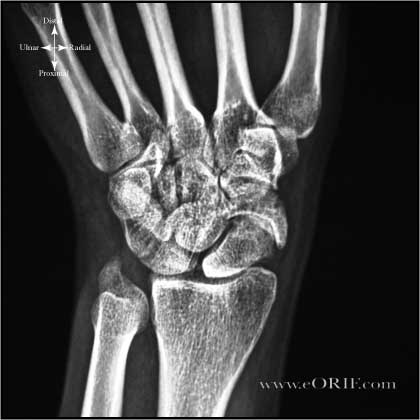
Scaphoid Nonunion Xray / Diagnositc Tests
- p/a, lateral wrist and scaphoid (p/a in ulnar deviation) and oblique 45-60 degree pronation views
- look for arthritis, cyst formation, bone resorption
- on lateral view a scapholumate angle >60 or a radiolunate angle >30 indicates DISI
- CT scan in the sagittal plane of the scaphoid is useful to quantify cortical healing and pre-op evaluation.
- height-to-length ratio on sagittal plane CT >0.65 corrresponds to significant scaphoid collapse.(Bain, J Hand Surg 23A:76, 1998)
- MRI useful pre-op to vascularity especially with waist fx and prox pole fx’s. MRI with gadolinium will demonstrate low signal intensity in T1 and T2 images in avascular areas. (Perlik PC, J Hand Surg Am 1991;16:479), (Trumble TE, J Hand Surg 1990;15A:557).
Scaphoid Nonunion Classification / Treatment
- cast and pulsed electromagnetic fields =69% union(Adams, J Hand Surg 17A:910, 1992
- avascular Proximal pole nonunion use dorsal approach
- Waist nonunion use volar approach
- >90% union with ORIF and bone grafting(vascularized bone grafting if avascular)
- Viable proximal pole fx=volar approach, incision over FCR extending distal over glaborous skin border of thenar eminence. Open FCR sheath, Incise floor of FCR sheath exposing prox pole. Preserve radioscaphocapitate ligament. K-wire joysticks reduction, bone graft, Remove volar lip of trapezium to allow proper longitudinal screw placement. Screw inserted over guide wire from distal to proximal.
- Avascular proximal pole fx=Dorsal approach. Midline longitudinal incision center on radiocarpal joint. 3rd extensor compartment entered and incised to enter joint. 4thcompartment and capsule reflected exposing scapholunate articulation. Debride nonunion. Flex wrist to visualize entery point adjacent to scapholunate interosseous ligament. Insert guide pin, measure, drive guidepin into trapezium, +/- derotation wire.
- Prox pole vascularized graft-relies on blood supply from 1,2 intracompartmental supraretinacular artery (1,2 ISRA)—(Zaidemberg, J Hand Surg 16A;474, 1991)
- salvage procedure = radial styloidectomy, proximal row carpectomy, limited intercarpal fusion, complete wrist fusion
Scaphoid Nonunion Associated Injuries / Differential Diagnosis
- Preiser's Disease
- Scaphoid fracture
- Scaphoid nonunion
- Keinbock's disease
- Ulnocarpal impaction syndrome
- SNAC
- SLAC
Scaphoid Nonunion Complications
- Nonunion
- Malunion
- Scaphoid subsidence or shortening with secondary screw penetration
- Neurovascular injury (cutaneous nerve, radial artery)
- Incorrect placement of a fixation screw
- Failure to recognize concomitant injuries.
Scaphoid Nonunion Follow-up Care
- Post-op: Place in volar thumb spica splint.
- 7-10 Days: If rigid fixation in good bone was achieved start controlled motion program with a removable splint and range-of-motion and gripping exercises.
- 6 Weeks: Consider CT to determine when union has occurred. Unprotected activity is not allowed until bridging bone is seen
- 3 Months: Consider bone stimulator if unionnot confimed
- 6 Months: assess ROM
- 1Yr: follow-up xrays, assess outcome
Scaphoid Nonunion Review References
- Trumble, JAAOS 11:380, 2003
- Greens Hand Surgery
|

