|
|
synonyms:greater tuberosity fracture, proximal humerus fracture
Greater Tuberosity Fracture ICD-10
Greater Tuberosity Fracture ICD-9
- 812.03(fracture of humerus, upper end, greater tuberosity; closed)
- 812.13(fracture of humerus, upper end, greater tuberosity; open)
Greater Tuberosity Fracture Etiology / Epidemiology / Natural History
- Greater tuberosity fractures which are displaced >5-10mm either superiorly or posteriorly can lead to painfull malunions with loss of function.
Greater Tuberosity Fracture Anatomy
- Greater tuberosity = insertion of supraspinatus, infraspinatus, and teres minor tendons
- Displaced greater tuberosity Fracture is pathognomonic of a longitudinal tear in the rotator cuff at the rotator interval between the supraspinatus and subscapularis tendons.
- Greater tuberosity fragment is pulled superiorly by the supraspinatus / infraspinatus. If displaced >5mm into the subacromial space a mechanical block to abduction and forward elevation can occur. Fragment may also be pulled posteriorly by the teres minor and infraspinatus which can lead to contracted external rotators and posterior capsule.
- Primary blood supply to humeral head=ascending branch of anterior humeral circumflex artery which runs in bicipital groove supplies.(Jaberg, JBJS 74A:508;1992)
Greater Tuberosity Fracture Clinical Evaluation
- Generally complain of shoulder pain after a fall.
- Swelling and ecchymosis in shoulder which can expend into chest wall and down arm.
- Point tenderness in the area of the greater tuberosity.
- Document NV exam, especially axillary n.
Greater Tuberosity Fracture Xray / Diagnositc Tests
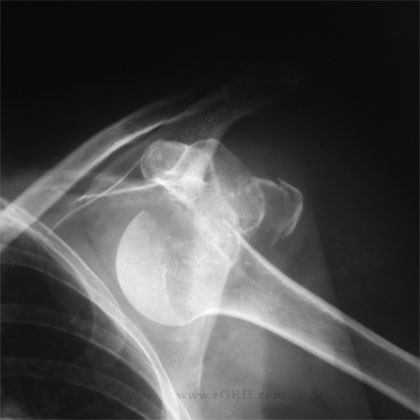
- A/P of glenohumeral joint, scapular Y, axillary. Greater tuberosity fragments are usually displaced either superiorly or posteriorly.
- CT helpful to identify exact location of greater tuberosity fragment and its donor site.
- MRI should be consider if a very small fragment is associated with marked weakness of the rotator cuff. Very small fragments can be associated with large RTC tears.
Greater Tuberosity Fracture Classification / Treatment
- Nondisplaced / Minimally displaced ( <5mm displacement): Sling, start PT within 2 wks for passive ROM only. Start strengthing, active ROM after fracture union is evident.
- Displaced (displaced >5mm, >3mm in active patients involved in frequent overhead activity): Open vs arthroscopic fixation (Flatow JBJS 73A 73:1213;1991). Tuberosity malpositioning >5mm significantly increases increases required abduction forces (Bono CM, JBJS 2001;83Br:1056), and can result in a mechanical block to shoulder abduction or external rotation and altered rotator cuff mechanics, causing weakness
- Displaced avulsion fracture: double row or suture bridge construct.
- Split fracture: ORIF with plate and suture fixation.
- Depression fracture: generally stable = non-operative treatment. Consider MRI to r/o rotator cuff tear.
- Greater tuberosity fracture associated with anterior shoulder dislocation: The glenohumeral joint should be reduced ASAP. Greater tuberosity fractures are then treated based on the amount of displacement seen on post-reduction xrays. Follow closely as fractures undisplaced after glenohumeral reduction frequently displace over time. ( Hebert-Davies, JOT 2015)
Greater Tuberosity Fracture ORIF Technique
- Pre-operative antibiotics
- General endotracheal intubation +/- scalene block
- Beach chair position, all bony prominences well padded
- Examination under anesthesia of shoulder
- Prep and drap in standard sterile fashion
- Anterolateral incision similar to that for a mini-open RTC repair.
- Deltoid muscle is at junction of anterior and lateral deltoid. Can is taken to ensure the deltoit split does not extend >5cm from the acromion to avoid injury to axillary nerve. If split is >4cm place a stay suture in the deltoid to prevent propagation during retraction.
- Subacromial bursectomy
- Identify fracture and donor site, irrigated / debride
- Several stay sutures are placed tinto the tuberosity fragement at the RTC insertion to aid in retraction and reduction
- Fracture is reduced and fixed with 4.0mm cancellous screws and washers, or #5 non-absorbable suture depending on fracture size and comminution. All holes in the greater tuberosity should be drilled to ensure no further fragment cominution occurs.
- Repair rent / close the rototar interval.
- Consider doing acromionplasty depending on PT age and acromial shape.
- Evaluated fracture stability through a ROM.
- Irrigate
- Close in layers.
Greater Tuberosity Fracture Associated Injuries / Differential Diagnosis
- Axillary nerve palsy
- Musculocutaneous nerve palsy
- Axillary artery injury
- Rotator cuff tear
- Shoulder Dislocation
- Bankart lesion: young athletes with anterior dislocations and greater tuberosity fractures can have associated Bankart lesions which generally require repair.
Greater Tuberosity Fracture Complications
- Malunion: Superiorly displaced malunions can produce a painful block to forward elevation. Posteriorly displaced malunions can produce a painful block to external rotation.
- Hardware failure
- Stiffness / Adhesive capsulitis
- Pain
- Nonunion
- Infection
- Rotator cuff tear (15%-30%), proximal migration
- Bursitis
- Heterotopic ossification
- Glenoid DJD
Greater Tuberosity Fracture Follow-up Care
- Patients are placed in a shoulder immobilzer with an abduction pillow (Ultrasling) post-operatively. Pendulum, elbow, wrist, hand ROM is started immediately.
- F/U at 7-10 days to remove sutures, check xrays and start passive ROM in physical therapy.
- Active ROM and strengthening are started after xray evidence of fracture healing.
- Return of ROM and strength can take 6months to 1 year.
- Shoulder outcome measures.
Greater Tuberosity Fracture Review References
- Rouleau JAAOS 2016
- Masters Shoulder
- George MS. Fractures of the greater tuberosity of the humerus. J Am Acad Orthop Surg. 2007 Oct;15(10):607-13
- °
|


